[This information guide is also available as a PDF to download.]
Treatment for early breast cancer usually includes surgery to the breast. This is normally combined with surgery to remove some or all of the lymph nodes (‘glands’) in the armpit. Other treatments, such as chemotherapy, radiotherapy and hormonal treatments, are sometimes recommended in combination with surgery.
Most women with early breast cancer can be treated with either:
- Breast conservation — surgery to remove the cancer and some normal tissue around it (wide local excision).This is almost always combined with radiotherapy(radiation treatment).
- Mastectomy — surgery to remove the whole breast. Radiotherapy is sometimes required after a mastectomy.
Each of these treatments has advantages and disadvantages. Some women have a preference for one treatment over another. Sometimes there are things about your breast cancer or your breast shape that will make your doctor recommend one treatment over the other. For example, if you have a large cancer or if the cancer affects more than one area in your breast, it may not be possible to remove all the cancer without a mastectomy.
What is breast conservation?
Breast conservation involves surgery to remove the breast cancer, which is usually followed by a course of radiotherapy to the breast. During surgery, some normal tissue around the cancer is also removed to reduce the chance of cancer being left behind.
The breast itself remains, though it may look slightly different. In some cases, removal of the cancer can be combined with a breast reduction or a breast lift, on one or both breasts. In other cases, tissue from the surrounding chest wall can be rotated into the area where the cancer was removed to create a more natural shape (so-called local perforator flap).
What are the advantages of breast conservation?
Breast conservation has some advantages compared to mastectomy:
- Your breast is left in place, keeping as much of your natural shape as possible.
- Your appearance will not be changed as much as it would be following a mastectomy.
What are the disadvantages of breast conservation?
Some of the disadvantages of breast conservation include:
- Your breast will look different after treatment. How different it looks depends on the size and location of the cancer, and the size and shape of your breast. Your treated breast may be slightly larger and heavier than your other breast or it may become smaller over time. This is due to a combination of the surgery and radiotherapy and the effect is difficult to
predict. - Your breast may feel different. Some women experience numbness or sharp shooting pain in the breast. This can be a nuisance but is not dangerous. It usually improves over the months and years after treatment.
- You may also lose some sensitivity in your nipple.
- Radiotherapy is almost always recommended after breast conservation surgery. Radiotherapy treatment involves going to the hospital for about three weeks of daily treatment. If your local hospital does not have a radiotherapy department you may need to travel to a hospital with one.
- You will need to have a mammogram of both breasts every year (and sometimes an ultrasound as well).
- The cancer can come back in the breast, although the risk is low (about 0.5% per year). Some women find this possibility causes them concern. However, the type of breast surgery you have will not significantly impact your survival after breast cancer. Mastectomy does not lead to better survival.
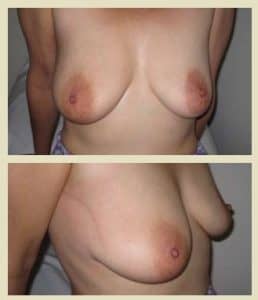
Figures 1a and 1b- This woman was treated with breast conservation (wide local excision and radiotherapy) for cancer in her right breast
Radiotherapy
Radiotherapy treatment is almost always recommended after breast conservation surgery. Radiotherapy is high-energy X-ray treatment. It is given to the remaining breast tissue after wide local excision, once the surgical wound has healed. The aim is to destroy any remaining cancer cells in the breast and reduce the risk of cancer coming back in the breast in the future. A usual course of radiotherapy involves a short treatment each day, five days a week, for about three weeks.
Most people tolerate radiotherapy well, however, there are some side effects. The most common side effects are fatigue, skin reddening (like sunburn) and irritation. These usually disappear about two weeks after the treatment has finished. Breast tenderness and tightness and swelling may take longer to improve.
More information about radiotherapy can be found in the Westmead Breast Cancer Institute’s Radiotherapy brochure.
What is mastectomy?
Mastectomy (also called total or simple mastectomy) is an operation to remove the whole breast, including the nipple. The chest muscles behind the breast are not removed. After the operation, the chest wall appears flat and there is a single scar where the breast was. You may choose to have a breast reconstruction at the same time as your mastectomy or at a later stage. More information about breast reconstruction is given later in this brochure.
What are the advantages of mastectomy?
Although a mastectomy is a bigger operation than breast conservation surgery, it has some advantages when compared to breast conserving surgery, these include:
- In some cases, radiotherapy is not required after surgery, but this depends on the individual and the type of cancer.
- Women who have a mastectomy tend to worry less about cancer coming back than women who have breast conservation treatment.
- You will no longer require a mammogram or ultrasound to the treated side. The other breast will still need to be checked each year with a mammogram and ultrasound.
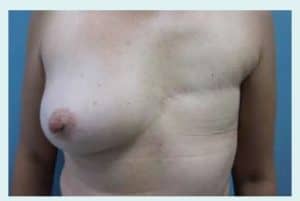 Figure 2 This woman had a mastectomy and did not have breast reconstruction. She wears an external prosthesis in her bra.
Figure 2 This woman had a mastectomy and did not have breast reconstruction. She wears an external prosthesis in her bra.
What are the disadvantages of mastectomy?
The disadvantages of mastectomy when compared to breast conservation
include:
- The whole breast is removed, leaving the chest flat. Some women find this quite upsetting and confronting. In most cases a breast
reconstruction is available either at the time of mastectomy or at a later time. It is also possible to wear a prosthesis in your bra if you choose not to have surgical reconstruction. - You may feel unbalanced after one breast is removed, especially if you have large breasts. In some cases you may be offered a breast
reduction on the other side to compensate for this. - Your stay in the hospital may be one to two days longer if you have a mastectomy rather than breast conservation surgery. This is because it is a bigger operation and there is usually a drain (plastic tube) in the wound to stop a build-up of fluid.
- There is a higher likelihood of developing a seroma (a collection of fluid under the arm or on the chest or breast) than after breast conserving surgery.
Breast reconstruction
Breast reconstruction is surgery to add shape to the body after a breast is removed (mastectomy). A reconstruction will not give you a new, normally functioning breast. Breast reconstruction is an option for most women who have a mastectomy.
It is usually possible to remove the breast tissue and leave most of the skin (‘skin sparing mastectomy’) and in some cases also the nipple (‘nipple sparing mastectomy’) depending on the body and breast shape and tumour type.
There are several options for breast reconstruction. It can be done using a breast implant or by using your natural body tissue. Breast reconstruction can be immediate (at the same time as mastectomy) or delayed (some time later).
You can ask your surgeon what option is most suitable for you.
More information about breast reconstruction can be found in the Westmead Breast Cancer Institute’s Breast Reconstruction brochure.
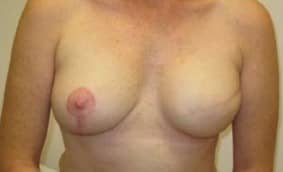
Figure 3- This woman had a left mastectomy and reconstruction using a tissue expander and a breast implant. She also had a breast lift on the right side to balance the breast size and shape.
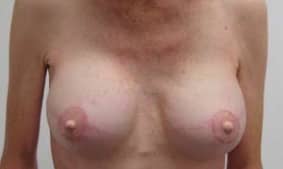
Figure 4- This woman had both breasts removed because she developed a cancer and also had a high genetic risk of breast cancer. She has undergone an artificial (implant) reconstruction with nipple reconstruction
What are the side effects of surgery for breast cancer?
All operations can have potential consequences and complications. However, complications are relatively uncommon in breast cancer surgery. The side effects are similar for breast conservation and mastectomy and can include:
- Pain after the operation – this is usually controlled with common pain
killers such as paracetamol with or without codeine. - Bleeding which requires a second operation to control.
- Infection in the wound.
- Painful scarring, called keloid scarring
- Seroma (a fluid build up) may need to be drained through a needle if it develops.
- Side effects from the anaesthetic.
Breast conservation surgery may carry the additional side effect of:
- Swelling and pain in the breast that can last for many months after
treatment.
Mastectomy may carry the additional side effects of:
- Tingling or shooting pain where your breast was, which can last for six months or longer. This is known as ‘post-mastectomy pain syndrome.’
- A change in posture or balance due to the loss of breast weight. Wearing a prosthesis or having a breast reconstruction or breast reduction on the other side can improve this.
- Scar and fatty tissue in the armpit area (sometimes referred to as a ‘dog ear’) that becomes very prominent. If it is uncomfortable or interferes with your bra fitting well, a small operation at a later time can improve this.
What about the lymph nodes (sometimes called lymph ‘glands’)?
Usually, some lymph nodes are removed from the armpit at the same time as the operation on the breast. Sampling the lymph nodes in the armpit will help your doctors to decide if additional treatment, such as chemotherapy will be recommended after surgery. The three operations for sampling the lymph nodes.
- 1.Sentinel lymph node biopsy (removal of only a few nodes for testing).
- Axillary clearance (removal of all of the lymph nodes).
- Targeted Axillary Dissection (TAD), where typically up to four nodes are removed, including the sentinel node.
Sometimes your surgeon will recommend removing some lymph nodes from other areas, such as between the ribs or near the collarbone, as well as sampling the lymph nodes in the armpit.
Recommendations for treatment to the breast are separate to recommendations for treatment to the lymph nodes. For example, breast
conservation can be combined with sentinel node biopsy or axillary clearance, depending on the type of cancer.
This also means that if you are having a mastectomy it is not always necessary to remove all of the armpit lymph nodes.
More information about treatment for the lymph nodes can be found in the Westmead Breast Cancer Institute’s Sentinel Node Biopsy and Lymphoedema brochures.
What about treatment after surgery?
About one week after the operation, you will return to see your surgeon for your pathology results. Your surgical dressing will also be removed and the wound will be checked to ensure that it is healing as expected.
A pathologist will examine the tissue removed during the operation in detail. With the information from the pathology report, you and your doctor can talk about whether other treatments such as radiotherapy, chemotherapy or hormone therapy are needed. You might be recommended to speak to several cancer specialists to discuss your treatment options.
What is the right choice?
Sometimes your doctor will recommend a particular treatment for you. Often the decision between mastectomy and breast conservation comes down to your personal choice. Everybody is different and what is right for one person may not be right for another. You have time to make up your mind. A week or two will not make any difference to how the treatment works. You should take the time to understand your choices and feel comfortable with them.
Who can help?
Treatment for cancer can be a very unsettling experience. Please talk to your surgeon, breast care nurse or other health professional if you have any concerns. These experienced practitioners are available to help you.
Useful contacts/websites
| Cancer Australia | canceraustralia.gov.au |
| Cancer Council | cancer.org.au |
| Cancer Council Helpline | 13 11 20 |
| Breast Cancer Network Australia (BCNA) | 1800 500 258 bcna.org.au |
Version 4 – WSP 109 October May 2025
© Westmead Breast Cancer Institute
[This information guide is also available as a PDF to download.]
